Precision Medicine
Precision medicine is a newer way to find the right treatment for each patient based on cancer subtype.
Cancer subtypes are smaller groups that cancer can be divided into based on certain traits of the cancer cell. Doctors use biomarker testing to find your specific subtype of cancer. Biomarker test results show which treatment is likely to work best for you based on your specific cancer subtype. Finding the right treatment based on subtype is precision medicine.
This approach is a change from the past. For example, years ago, everyone with stage 3 lung cancer received the same treatment. It probably included some combination of surgery, chemotherapy, and radiation.
Today, doctors know more about cancer. They understand more about what causes cancer to grow and divide uncontrollably. They have learned that there is more to cancer than just the type and the stage. Doctors are now able to use information about what’s going on inside cancer cells to learn the best way to treat the disease.
Precision medicine is only available for certain types and stages of cancer.

What questions should you ask your doctor about biomarker testing?
Our worksheet "Talking About Biomarker Testing" can help.
Precision Medicine: Biomarker Testing
Biomarker testing helps your doctor understand what is unique about you and your cancer on a molecular level. A biomarker is a molecule in your body that your doctors can measure to tell them something specific about you and your cancer. Biomarkers…
Cancer Types and Subtypes
The type of cancer you have is usually named for the organ or tissues where the cancer forms. Common cancer types include breast, colon, prostate, skin, and lung.
The subtype provides more information about the cancer. It is based on certain traits of the cancer cell. There are many different subtypes of cancer, and new ones are being discovered all the time.
Some cancers have well-known subtypes. For example, you may have heard of triple negative breast cancer. Other cancers have subtypes that were just identified in recent years and are not as well known, like ALK-positive non-small cell lung cancer.
It is important to know the subtype of a cancer for treatment planning. Certain treatments work better for certain subtypes. Finding the right treatment based on subtype is precision medicine.

Understanding Genes, Mutations, and Biomarkers
To understand more about how precision medicine works, it helps to know a little about genes, mutations, and biomarkers.
What is Precision Medicine?
Ruby, your virtual community navigator, will help explain what you need to know about precision medicine and how it can impact cancer treatment.
Genes
Genes carry the information that pass on traits that can be inherited from parents to children. Genes affect the way our cells and bodies work. Genes are found inside of cells and made of DNA. Genes can:
- Carry traits, like eye color or height, from parent to biological child.
- Control how our body makes substances called proteins.
- Tell cells what to do, including when to grow and divide or when to stop growing and dividing.
Genes also hold clues to our health. In cancer, the genes and proteins that make up one person’s tumor can be very different from the genes and proteins of another person’s tumor. In other words, cancer genes vary from person to person. Genes can change. A change in a gene is a mutation. Some mutations can lead to cancer. There are 2 types of mutations: those that happen in our lifetime (acquired mutations) and those that are passed down through families (inherited mutations).
Acquired Mutations
Genetic mutations that develop during your lifetime are acquired mutations. They occur as you get older and are the result of the wear and tear of life, the environment around you, and sometimes, lifestyle choices. You do not inherit them from your parents and you cannot pass them on to children. Acquired mutations are not found in all your cells. Sometimes, there may be acquired mutations in just the cancer cells. They can affect how cancer grows and spreads. Acquired mutations can also be called biomarkers.
Inherited Mutations
A genetic mutation is a change in a gene. Mutations in your genes can be inherited from your parents and can be passed on to children. Your genes may be tested for mutations that increase your risk of getting cancer. You may hear them described as genes that cause cancer. In fact, it is the change or mutation in the gene — not the gene itself — that can increase the risk of cancer.
Biomarkers
A biomarker is a sign of disease or abnormal function that can be measured in your blood, tissue, or bodily fluid. In cancer, biomarkers are often used to help choose the best treatment for you. Biomarkers can be proteins, genes, or gene mutations. They have names. The name is usually a 3- or 4-letter abbreviation. Examples include HER2 in breast cancer or EGFR in lung cancer. Biomarkers tell your doctor about the subtype of the cancer in your body. Biomarkers in precision medicine can be used to:
- Help choose the best treatment for you.
- Judge how well your body would respond to a specific treatment.
- Predict your risk of developing cancer.
- Understand the makeup of your cancer and how it changes over time.
- Look for early signs of how well your body responds to a specific treatment.
Biomarker Testing
Biomarker testing provides more information about the cancer you have — beyond the type and stage. Health care providers who test for biomarkers are trying to find out if you have a cancer subtype that matches to a targeted therapy drug.
In some cancer types, targeted therapy drugs are only available for certain cancer subtypes, which are based on the biomarker information your doctor learns from comprehensive biomarker testing. They collect a sample of cancer cells from your blood or bodily fluids or from your tissue taken during surgery or biopsy. Your sample is sent to a lab for testing. The test looks for biomarkers in your cancer sample. The test results can be used to help guide your treatment options.
Health care providers use different names when referring to biomarker testing. You may hear it called:
- Comprehensive biomarker testing
- Gene-based cancer testing
- Genetic testing of the cancer
- Cancer marker testing
- Next generation sequencing
- Genomic profiling
- Mutation biomarker testing
- Genomic testing
- Molecular profiling
- Tumor marker testing
- Mutation testing
- Molecular testing
These are all the same kinds of tests. Their results help your doctor know the treatments that might work best for you.

Find answers to common questions about biomarker testing.
Learn More About BiomarkersWhat Is a Targeted Therapy Drug?
Targeted therapy drugs are a newer kind of cancer treatment. They work differently from other treatments. They treat cancer with less harm to cells that are not cancer. This is because they are better able to attack your cancer cells and leave healthy cells alone.
Targeted therapy drugs can work in several ways:
- They can find cancer cells.
- They can destroy cancer cells directly.
- They can stop cancer cells from growing uncontrollably.
- They can cut off the blood supply that tumors need to grow and survive.
Targeted therapies may be given alone or in combination with chemotherapy or other treatments. These drugs “target” specific cancer subtypes. They are only likely to work in those subtypes.
What Is a Targeted Therapy Drug?
Ruby, your virtual community navigator, will help you understand what targeted therapies drugs are, how they work, and if targeted therapy is an option for you. Have a concern of your own? Please call our Cancer Support Helpline to talk with an…
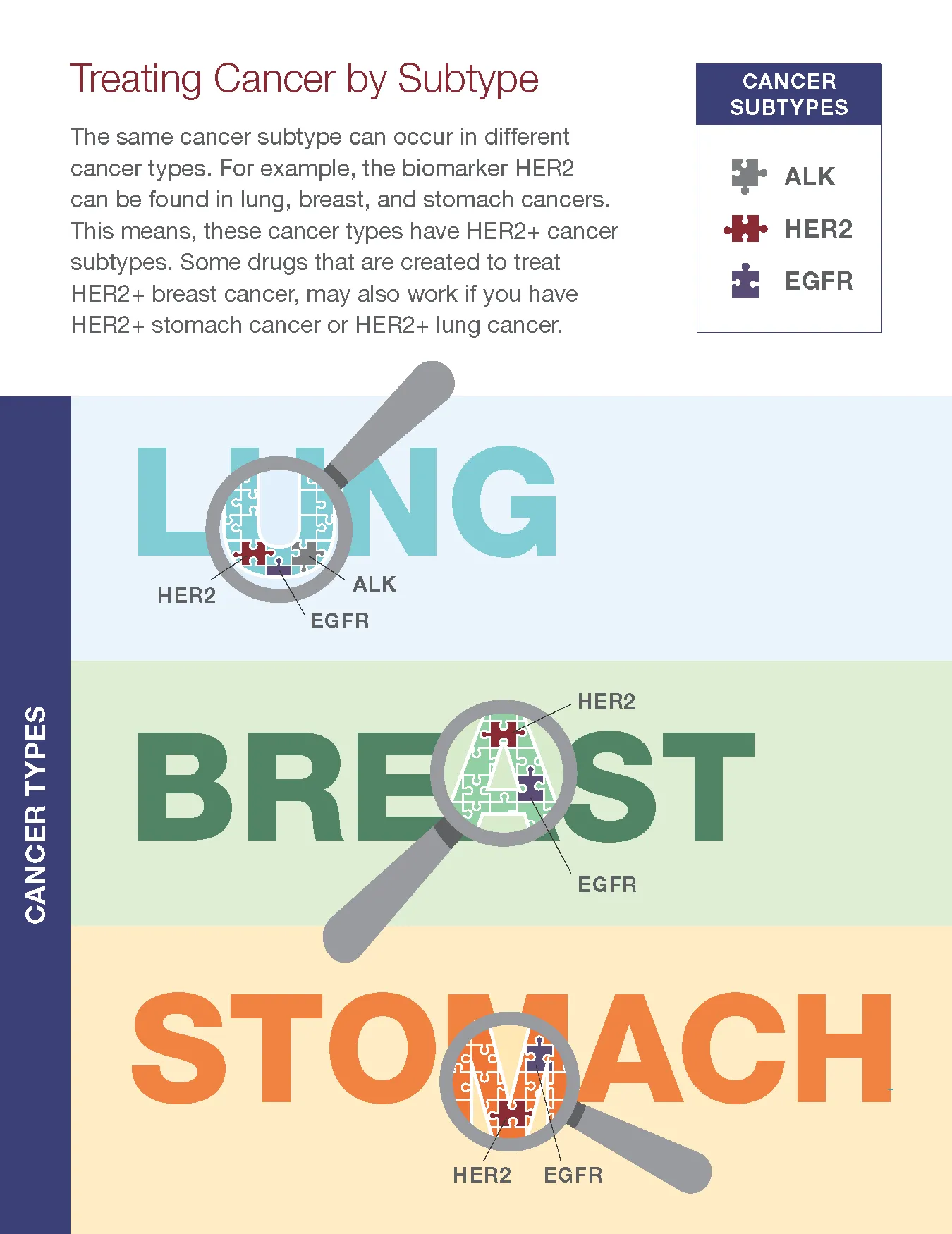
Treating Cancer by Subtypes
The newest way to treat cancer is based on cancer subtype, rather than just type of cancer. Biomarker testing is used to find subtypes which are typically given a 3- or 4-letter abbreviation. The subtype provides more information about what is going on inside of a cell that may be causing the cancer to grow and spread.
Some treatments are approved for any cancer with a certain subtype. Different types of cancer (like breast cancer and stomach cancer) can share the same subtype. Breast cancer and stomach cancer both have HER2+ subtypes. For example, some drugs that are created to treat HER2+ breast cancer might also work if you have HER2+ stomach cancer.
Some key things to know about treating cancer by subtype are:
- Some drugs that treat cancer based on subtype are approved by the FDA. Many more are available through clinical trials.
- Treating cancer by subtype is not routine everywhere. Some cancer centers do not have the labs to run biomarker testing needed to learn subtypes. Some doctors are less familiar with this approach to treatment.
Genetic Testing
Genetic testing can help you learn more about your cancer risk and look for changes (mutations) in your genes. The results might tell you more about your chance of getting certain cancers in your lifetime.
Genetic testing may be offered or recommended either because:
- You have cancer. If you have cancer, your doctor may test to see if you inherited a mutation that increased your risk of developing this cancer. This may be called “genetic testing for an inherited mutation.”
- Your family history suggests that you may be at high risk of developing cancer. If you do not have cancer, a doctor or genetic health care professional may recommend testing to see if you inherited a mutation that increases your risk of getting cancer. This may be called “genetic testing for inherited cancer risk.”
Genetic Testing for Inherited Cancer Mutations
In some cases, cancer runs in families. It seems to be passed down from parents to children. You may have heard this called “inherited cancer,” but this is not correct. What is inherited is a change in a gene — a mutation. The mutation in the gene increases a person’s risk of cancer. This is called inherited cancer risk. It is not the cancer itself that is inherited. If you have cancer, doctors may test your genes to see if you inherited a mutation. The results of genetic tests may also help your doctor choose the right treatment option for you. Doctors do not test every patient for inherited mutations. The decision to do so may depend on:
- The type, stage, or other characteristics of your cancer.
- Your personal health history.
- Your family health history.
- Your age, race, or ethnicity (some inherited cancers are more likely to affect people in certain groups or who develop cancer at younger ages).
- Whether the test results will affect your treatment options.
In some cases, your doctor may not offer this test even though it would be helpful. Talking with a genetics professional can help you understand whether this testing is needed. About 5% to 10% of all cancer cases occur in someone who inherited a genetic mutation that increases cancer risk.
Genetic Testing for Inherited Cancer Risk
Genetic testing is not just for people with cancer. Some people are concerned about cancer based on their family history. In this situation, it is best to talk with a health care provider or a genetics professional. They may recommend testing to see if an inherited mutation increases a person’s risk of getting cancer. This is called “genetic testing for inherited cancer risk.” They will ask about the relatives who have had cancer, how old they were at diagnosis, and the types of cancer they had.
Genetic Testing vs. Biomarker Testing
Precision medicine can involve 2 types of tests:
- Tests for inherited genetic mutations that increase your risk of cancer.
- Tests for biomarkers that drive your cancer to grow.
These tests are sometimes confused. This happens in part because people use different words or sometimes the same words to describe them.
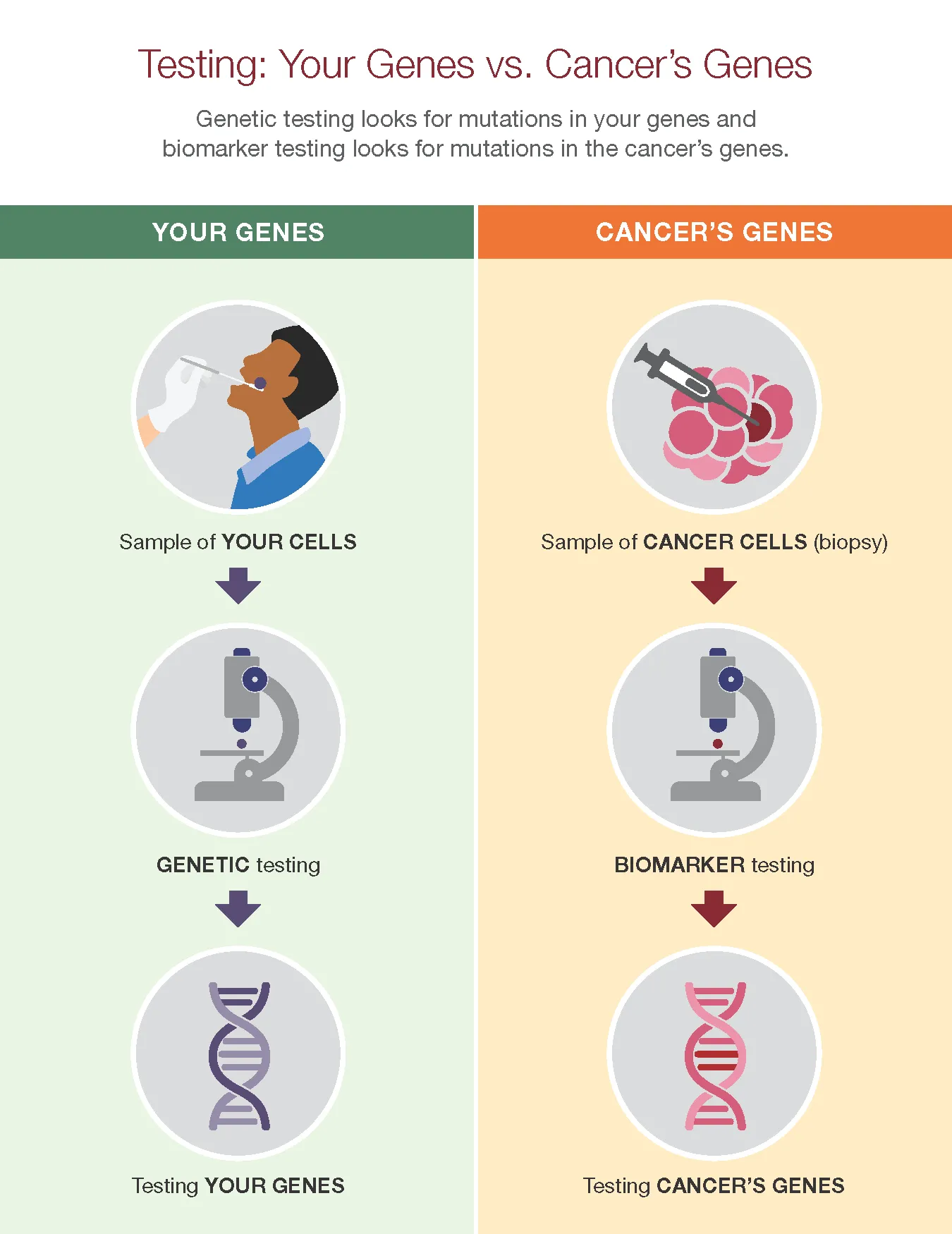
Genetic testing looks for mutations in your genes and biomarker testing looks for mutations in the cancer’s genes. Comprehensive biomarker testing is used to find the subtype of cancer. The results of these tests offer more information about a person’s cancer. Genetic testing is most often used to find an inherited mutation or inherited risk.
Testing for Blood Cancers
Gathering as much information as you can about your cancer will help you work with your health care team to make informed decisions.
Measurable residual disease (MRD) testing is used in blood cancers such as:
- Acute lymphoblastic leukemia (ALL)
- Acute myeloid leukemia (AML)
- Chronic myeloid leukemia (CML)
- Lymphomas
- Multiple myeloma
Together, you and your doctor can make the best decisions about your blood cancer treatment using the knowledge gained from MRD testing. MRD levels help your doctor determine how well your blood cancer treatment is working. It also helps predict the risk of your cancer returning. Checking MRD can also help confirm and monitor remission.
Understanding MRD
Even if you’ve had cancer treatment such as chemotherapy and have reached remission, a small number of cancer cells can remain in your body. This is called MRD. It is sometimes referred to as minimal residual disease. These cancer cells may not be detected through normal lab tests, and you may not show any signs or symptoms of cancer.
MRD testing is so powerful because it can detect 1 cancer cell in 100,000 healthy cells. It may even be able to detect 1 cancer cell in 1 million healthy white blood cells. Understanding how much MRD you have gives you and your doctor insights about how your body is responding to treatment. This form of personalized medicine allows treatment to be tailored to your unique needs. People without MRD may live longer without disease than those with MRD.
Types of MRD Tests
Three types of tests are available to assess MRD. The testing method is determined by the type of blood cancer you have. The main tests for MRD are:
- Flow cytometry, which is performed using a bone marrow sample. Flow cytometry can find 1 cancer cell in 100,000 healthy bone marrow cells. Results are usually available in less than 1 day.
- Polymerase chain reaction (PCR), using either a blood sample or a bone marrow sample to recognize DNA specific to cancer cells. PCR can find 1 cancer cell in 100,000 to 1 million healthy bone marrow cells. Results may take several weeks.
- Next-generation sequencing (NGS), which requires a bone marrow sample to examine the DNA or RNA of cells for patients living with ALL. NGS is the most sensitive of the 3 tests. NGS can find 1 cancer cell in 1 million healthy bone marrow cells. Results are usually available within 1 week.
Managing Costs
The cost of genetic and biomarker testing varies. In some cases, the costs may be covered by insurance. Whether it is covered will depend on the reason for testing, the test being done, and the insurance policy. If you cannot afford the cost of the tests, assistance may be available. Talk with your health care team about the cost and how to pay for it. Ask if your insurance will cover the testing. For more help on coping with cancer costs, call 844-792-6517.
Would you like a print copy of these educational materials?
We can mail our Frankly Speaking About Cancer pieces to you. Shipping is free for up to 20 pounds.






