Metastatic Breast Cancer
Table of Contents
Breast cancer starts in the ducts or lobules of the breast. Metastatic breast cancer means that breast cancer has spread to other parts of the body. It is also called stage IV (4) breast cancer. When breast cancer spreads, it most commonly spreads to the bones, lungs, liver, and brain.
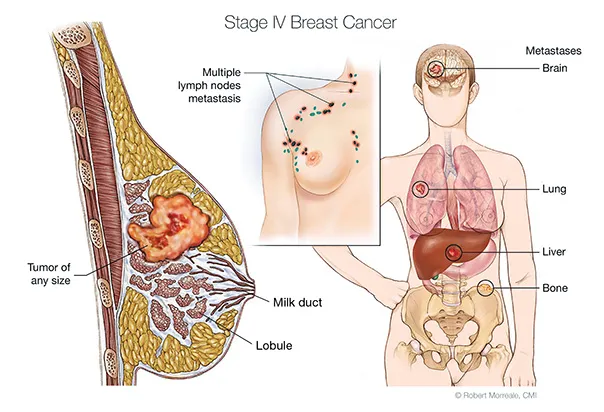
Metastatic breast cancer can be a new cancer. Or it can be the return of a prior breast cancer. If you have breast cancer for the first time and it has already spread, it is called de novo metastatic breast cancer.
Even though the cancer may be in a different part of the body, it is still breast cancer. This is true even if your breasts were removed. This means that breast cancer treatments, not treatments for other cancers, will work best.
If you have been treated for breast cancer in the past and develop a new growth or cancer in a different part of the body, your doctor may perform tests to confirm if the cancer has recurred. The most common sites for breast cancer to spread to are the bones, lungs, liver, lymph nodes, adrenal gland and brain. If your cancer spreads to the brain, MBCBrainMets.org has more information.
Treatment Options & Side Effects
Treatment options for breast cancer depend on the cancer stage, cell type, and the person’s age and general health.
Breast Cancer Types
There are three major types of breast cancer that can become metastatic:
- Invasive ductal breast cancer – This type forms in the ducts of the breast. The ducts are the tubes that carry milk. This type may appear as a lump you can feel. It is the most common type.
- Invasive lobular breast cancer – This type forms in the glands or lobules of the breast.
- Inflammatory breast cancer – This is a rare form of breast cancer. It may appear as a rash.
Subtypes
Your doctor will want to know as much about your cancer as possible. This means knowing the subtype. The subtype is based on biomarkers. Biomarkers are signs in your blood or tissue. They help describe your cancer. Your cancer will be tested for:
- Hormones: Breast cancer can be estrogen receptor positive (ER+) and/or progesterone receptor positive (PR+). This means that hormones play a role in the cancer, and the cancer may respond to anti-estrogen hormone therapy.
- HER2: Breast cancer can be HER2/neu positive (HER2+). This means that a protein called human epidural growth factor receptor 2 (HER2) is present in the cancer. These cancers may be treated with targeted therapy.
If the cancer is negative for both hormones and HER2, it is called triple negative breast cancer. There are fewer treatments that work against this subtype of cancer. Doctors are working hard to understand it better and find effective ways to treat it.

Coping With Triple Negative Breast Cancer?
Learn about 3 key areas where you may need extra support, and resources that can help.
Quick Guide to Metastatic Breast Cancer
This video provides an overview of metastatic breast cancer (MBC). This video covers MBC diagnosis, subtypes, treatments, genetic testing, talking with your health care team, and more. Click here to learn more about MBC.
Diagnosis and Treatment Planning
A complete diagnosis usually takes more than one doctor’s visit. It may involve scans, blood tests, and a biopsy. Your doctor will work with a team to figure out:
- If you have breast cancer or another kind of cancer
- The type and subtype of breast cancer
- The places in your body it has spread
If you had breast cancer in the past, your doctor will confirm whether it is the same type of breast cancer as before. Breast cancer that has spread to another part of the body is still breast cancer. The site(s) where the cancer is found may affect your treatment options.
Treatment Planning
The process of learning about treatment options and choosing one is called treatment planning. You will be asked to make choices at the start of treatment and again along the way. Here are some steps you can take to feel more in control and better able to make decisions that are right for you.
- Find the right healthcare team for you.
- Learn how to work with your team.
- Understand the goals of treatment.
- Choose the right treatment for you.
Look for a doctor with expertise in metastatic breast cancer. Consider communication style, approach to treatment, location, insurance, and the availability of clinical trials, among other factors.
Keep a list of questions. Ask about the best way to get answers to your questions. Bring a friend or family member to visits to listen and take notes. Tell your team about any symptoms or side effects.
Treatment for metastatic breast cancer is very different from treatment for early-stage breast cancer. After breast cancer has spread to other parts of the body, treatment needs to focus on the whole body. These whole-body treatments are called systemic therapies.
Ask questions about each possible treatment. Ask about the goal of the treatment. What are the possible side effects, and how will they be managed? Think about what is most important to you. Share your wishes with loved ones and your healthcare team.
Finding Joy in Metastic Breast Cancer (MBC) Diagnosis
Felicia, who lives with Metastatic Breast Cancer (MBC), discusses finding joy through her cancer journey.
Getting a Second Opinion
Many people find that it helps to get a second or even third opinion from another oncologist or cancer center. Talking with a second doctor can help you better understand your disease and how to treat it. Ask your doctor for suggestions of someone to see for a second opinion. Or, use these resources:
Diagnosis: Metastatic Breast Cancer (MBC)
Mary Lou, who lives with MBC, discusses her diagnosis and learning to cope with it.
Treatment and Side Effects
The goal of treatment for metastatic breast cancer is to slow down or stop the growth of cancer. Or, the goal may be to help you feel better. People often try different treatments, staying with one for as long as it works. Your doctor may recommend 1 or more therapies. They all have different side effects. Ask about the side effects of the treatments you consider.
Know Your Biomarkers
Knowing the biomarkers of your breast cancer helps doctors decide how to treat it. The 3 most important biomarkers are:
- ER, the hormone estrogen
- PR, the hormone progesterone
- HER2, the protein HER2 (her-two)
Your cancer can be positive (+) or negative (-) for them.
This table shows the possible treatment options based on these 3 biomarkers. If you know the biomarkers of your breast cancer, check this table to see which treatment options apply to you.

Review Your Treatment Options
There are 5 main approaches to treating metastatic breast cancer. They may be used alone or in combination.
These drugs block hormones that drive cancer growth. It is used to treat breast cancers that are ER+ or PR+. You may take other treatments at the same time as these drugs.
Chemotherapy uses drugs to destroy or damage fast-growing cells like cancer cells. It is used to shrink tumors, slow cancer’s growth, relieve symptoms, or help people live longer. You may get one type of chemotherapy at a time (single-agent therapy) or several drugs in combination (combination therapy). You also may get chemo in combination with other types of treatment.
These drugs target specific changes in cancer cells that help them grow, divide, and spread. They treat the cancer cells with less harm to normal cells. There are different types of targeted therapy. You may get targeted therapy alone or in combination with other treatments, like chemotherapy.
This is a type of cancer treatment that uses the body's natural defenses (the immune system) to identify, attack, and kill cancer cells. Immunotherapy is used for triple negative breast cancer (TNBC) that is PD-L1 positive.
Be sure to ask about clinical trials. These are studies to test new treatments or learn how to use current treatments better. They may be the only way to try a promising new treatment. Many people with metastatic breast cancer get their treatment through a clinical trial.
Other treatments such as surgery or radiation therapy may help with symptoms or side effects. They are not generally used to treat metastatic breast cancer. Palliative care can also help treat symptoms and side effects. It does not treat the cancer itself.
Managing Side Effects
Coping with the side effects of treatment can be one of the hardest parts of cancer. It can be scary to read through long lists of side effects. This can be especially upsetting when you think about being in treatment off and on for the rest of your life. It helps to plan in advance and talk with your healthcare team.
Before you start treatment, ask your healthcare team about the side effects of the treatment you are considering. Find out how to manage them.
After you start treatment, keep track of how you feel. Write down when you notice a problem, how long it lasts, and if there is anything that makes it better. Let your healthcare team know.
Keep in mind:
- You probably won’t have all the symptoms or side effects you read on a list.
- Your healthcare team can help you manage symptoms and side effects.
- Your healthcare team only knows what you tell them.
Common side effects may include:
Hormone therapy – Hot flashes, vaginal discharge or dryness, post-menopausal symptoms, joint stiffness, weight gain, and pain or soreness at the injection site.
Chemotherapy – Nausea and vomiting, fatigue, hair loss, mouth sores, cognitive changes, low blood counts, numbness or tingling in the feet, nail and skin changes, diarrhea, loss of appetite, and skin rash.
Targeted therapy – Skin rash, diarrhea, fatigue, mild nausea and vomiting, low blood counts, hair loss, mouth sores, abnormal liver or blood tests, and risks for bleeding.
Quick Guides on Managing Side Effects of MBC Treatment
Quick Guide on Metastatic Breast Cancer Symptoms and Side Effects
This video highlights common symptoms and side effects that patients living with Metastatic Breast Cancer (MBC) may experience. It covers talking to your health care team, treatment to manage side effects, finding support, coping with costs, and more.
Quick Guide on Hair Loss for Metastatic Breast Cancer Survivors
This video covers the side effect of hair loss that patients living with Metastatic Breast Cancer (MBC) experience as a result of some chemotherapy treatments. It includes the basics of hair loss, how to prepare for it, and talking to your health care team about hair loss.
Quick Guide on Bone Loss or Weakness for Metastatic Breast Cancer Survivors
This video covers the side effect of bone loss or weakness that patients living with Metastatic Breast Cancer (MBC) may experience. It includes the causes of bone loss or weakness, tips for coping with bone loss or weakness, and talking to your health care team about bone loss or weakness.
Quick Guide on Cognitive Changes for Metastatic Breast Cancer Survivors
This video covers the side effect of “chemo brain” that patients living with Metastatic Breast Cancer (MBC) may experience during treatment. Chemo brain is characterized by brain fog and difficulty concentrating. The video includes what chemo brain is, tips for coping, and talking to your health care team about chemo brain.
Quick Guide on Nerve Problems for Metastatic Breast Cancer Survivors
This video covers the side effect of pain and neuropathy that patients living with Metastatic Breast Cancer (MBC) may experience. It includes what is described as pain, types of treatment medication, how to cope with pain, what neuropathy is, and how one can cope with neuropathy. Additionally, there are tips for talking to your health care team about pain and neuropathy.
Quick Guide on Fatigue for Metastatic Breast Cancer Survivors
This video covers the side effect of fatigue that patients living with Metastatic Breast Cancer (MBC) may experience. It includes what fatigue is, the causes of fatigue, how to cope with fatigue, and tips for talking to your health care team about fatigue.
Quick Guide on Lymphedema for Metastatic Breast Cancer Survivors
This video covers the side effect of lymphedema that patients living with Metastatic Breast Cancer (MBC) may experience. It covers what lymphedema is, how to cope with lymphedema, and tips for talking to your health care team about lymphedema as well as recommendations they may have.
Quick Guide on MBC Symptoms and Side Effects: Diarrhea and Constipation
This video covers the side effect of diarrhea and constipation that Metastatic Breast Cancer (MBC) patients may experience. It includes tips to alleviate discomfort of diarrhea and constipation, how to cope with diarrhea and constipation, and when to talk to your health care team about diarrhea and constipation.
Quick Guide on MBC Symptoms and Side Effects: Mouth Sores and Difficulty Eating
This video covers the side effect of mouth sores & difficulty eating that patients living with Metastatic Breast Cancer (MBC) may experience. It includes what mouth sores are, who is more prone to mouth sores, how to prevent them, tips for coping with them, and what foods to avoid when afflicted with sores. Additionally, there are tips for talking to your health care team about mouth sores as well as recommendations they may have.
Quick Guide on Skin and Nail Changes for Metastatic Breast Cancer Survivors
This video covers the side effects of nail changes, skin rashes, and sensitivities and hand foot mouth syndrome that patients living with Metastatic Breast Cancer (MBC) may experience. It explains nail changes, skin rashes, and sensitivities, as well as hand foot mouth syndrome, and includes tips for coping with each symptom.
Quick Guide on Hot Flashes and Vaginal Dryness and Discharge for Metastatic Breast Cancer Survivors
This video covers the side effects of hot flashes and dryness that patients living with Metastatic Breast Cancer (MBC) may experience. It includes what to do when hot flashes become uncomfortable, medications that treat hot flashes, symptoms of dryness or discharge, sexuality and sexual intimacy, and ways to cope. Additionally, there are tips for talking to your health care team about hot flashes and dryness, as well as recommendations they may have.
Quick Guide on MBC Symptoms and Side Effects: Stress, Anxiety, and Depression
This video covers the side effects of stress, anxiety, and depression that patients living with Metastatic Breast Cancer (MBC) may experience. It includes common emotions of cancer patients, signs of depression, signs of anxiety, suggestions for finding treatment, medication options, and active ways to combat stress and anxiety. Additionally, there are tips for talking to your health care team about stress, anxiety, and depression, as well as recommendations they may have.
Quick Guide on MBC Symptoms and Side Effects: Insomnia
This video covers the side effect of insomnia that Metastatic Breast Cancer (MBC) patients may experience. The video covers what insomnia is, ways to cope, and possible medications for short-term treatment.
Quick Guide on MBC Symptoms and Side Effects: Nausea and Vomiting
This video covers the side effects of nausea and vomiting that patients living with Metastatic Breast Cancer (MBC) may experience. It includes the different types of nausea, how to prevent nausea and vomiting, as well as possible diets to help with nausea and vomiting.
Quick Guide on Low Blood Count for Metastatic Breast Cancer Survivors
This video covers the side effect of low blood counts that Metastatic Breast Cancer (MBC) patients may experience. It includes the different types low blood counts, medications that increase the risk of bleeding, tips to prevent bleeding, and when to talk to your health care team.
Quick Guide on Symptoms of Bone Metastases for Metastatic Breast Cancer Survivors
This video covers the side effect of bone metastases that patients living with Metastatic Breast Cancer (MBC) may experience. It includes what bone metastases is, how to cope, diet and exercise recommendations, how to prevent falls, and when to talk to your health care team.
Tips for Coping With Metastatic Breast Cancer
Living with metastatic breast cancer isn’t easy. Some days will be better than others. It may help to know you are not alone. More than 150,000 people in the United States are living with metastatic breast cancer. While there is still no cure, people with metastatic breast cancer are living longer, fuller lives than ever before.
Metastatic breast cancer brings change. Change may affect any aspect of your life. What was once important to you may be different now. Treatment takes time and energy. Taking care of yourself physically and emotionally is a key concern. Relationships become more important.
As you try different treatments, your expectations for the future may change. You may have extended periods in and out of treatment. You may not know what to expect. Living with uncertainty may be one of the hardest things to accept.
Even if things are uncertain, you can find joy. Focus on what’s important to you. Have hope – even for small things, like a favorite food or time with a friend. Hopes can become short-term goals. They can give you energy to keep going, even when you are feeling down. Learn ways to cope with common concerns such as parenting, relationships, sexual intimacy, work, dating, and body image.
Finding the Support You Need
Don’t try to go through it alone. Reach out to others for help and support. It may take a while to find the support that is right for you, but don’t give up. You can:
- Talk with a cancer social worker, therapist, or spiritual advisor.
- Talk with friends or family members.
- Join a metastatic breast cancer support group.
- Participate in chat groups or discussion boards.
- Take part in community or faith-based activities.
- Attend an educational program for people with metastatic breast cancer.
- Advocate for support, services and research to help people with metastatic breast cancer.
Remember to take care of yourself. Eat healthy foods. Physical activity can lift your spirits. Exercise your mind and body through meditation or yoga. Try keeping a journal.
Caregiver Support
Caregivers help or arrange help for people who are ill or disabled. This help can take different forms. Some caregivers assist with money matters, insurance, household chores, rides, or making appointments. Caregivers may or may not live with the person.
Caring for someone who has cancer is not easy. Caregivers need support and help. If you are caring for a person with metastatic breast cancer:
- Find support. Share your feelings with others. Try a caregiver support group, either online or in person. Ask the hospital or cancer center if they have support groups for caregivers.
- Look for extra help. Ask family, friends, and members of your community if they can help. If they offer, give them specific tasks. If you can afford it, consider hiring people to help care for your loved one or help you with chores, childcare, or errands.
- Take breaks. Carve out time for yourself. Spend time with people important to you, and take time for activities you enjoy. Don’t feel guilty about making time for yourself—it is important for your own health.
- Take care of yourself. Caregivers are often very focused on their loved one. They may neglect their own health. Take time to sleep, exercise, and eat healthy foods.
- Learn about the Family and Medical Leave Act (FMLA). You may qualify to take up to 12 weeks of unpaid, job-protected leave to care for a seriously ill family member.
- Learn about financial assistance. You may miss days of work. You also may have high out-of-pocket costs from parking, transportation, and food as part of your caregiving duties. Ask the hospital if they can provide help with financial counseling for caregivers.
Costs and Expenses
Cancer can be expensive. The cost itself can be a burden, as can the stress it causes. It’s never too early to start to think about the cost of care.
Discuss the cost of treatment with your health care team. Even though it may be hard, starting open conversations early can help you in the long term. Ask for help from a trusted friend or family member, patient navigator, or social worker. As you think ahead, consider:
- Medical expenses, including prescription drug co-pays
- Missed time from work or a time when you won’t be able to work
- How caregiving may affect the earnings of a partner or other family member
- Childcare or transportation expenses
Medicare and Social Security Disability Benefits (SSDI)
People with metastatic breast cancer are eligible for Medicare and automatically qualify to receive disability from the Social Security Administration. To be eligible and earn Social Security Disability Benefits (SSDI), you must have been employed within the last 10 years and not able to work due to your disability.
Tips From Patients & Caregivers
Treatment: Metastatic Breast Cancer (MBC)
Marian, who lives with MBC, discusses her treatment with MBC.
Activity: Metastatic Breast Cancer (MBC)
Marian, who lives with MBC, discusses getting back to being active after treatments.
Tips: Metastatic Breast Cancer (MBC)
Mary Lou, who lives with MBC, shares her tips for living with MBC and the importance of having support.
Caregiving with Metastatic Breast Cancer
Felicia talks about MBC and caregiving.
Caregiving: Metastatic Breast Cancer (MBC)
Peter discusses being a caregiver for Jeana, who lives with MBC.
Support: Metastatic Breast Cancer (MBC)
Marian, who lives with MBC, discusses how she finds support through her cancer journey.
Finances and Jobs: Metastatic Breast Cancer (MBC)
Mary Lou, who lives with MBC, discusses the importance of talking to human resources about your diagnosis and how it will affect your life.
What Do I Tell My Kids: Metastatic Breast Cancer (MBC)
Jeana, who lives with MBC, and her caregiver Peter, discuss talking openly and honestly with their kids about her cancer.
Family: Metastatic Breast Cancer (MBC)
Jeana, who lives with MBC, discusses the changing family dynamics that come with a cancer diagnosis.
Grandkids: Metastatic Breast Cancer (MBC)
Marian, who lives with MBC, discusses talking honestly with her grandkids about her cancer diagnosis.
Frankly Speaking About Cancer Library
LibraryWould you like a print copy of these educational materials?
We can mail our Frankly Speaking About Cancer pieces to you. Shipping is free for up to 20 pounds.