Bladder Cancer
Table of Contents
Your bladder is a hollow muscle that stores urine until it is passed through the urethra, when you urinate.The bladder has 4 layers of tissue:
- The inside layer is the bladder lining.
- Next to that is connective tissue (that also has nerves and blood vessels).
- The third layer is the thick bladder muscle, which squeezes when you urinate.
- The outside layer is made up of fatty tissue.
Bladder cancer occurs when the cells in the bladder—like the cells in other parts of your body—grow and divide. If a normal cell collects too many genetic errors, it can turn into a cancer cell. As the cancer cell grows and divides, it will begin to form a tumor. This can cause bleeding or affect how your bladder functions.
Risk Factors
There are some risk factors for bladder cancer that you cannot control. These include:
- Being male
- Getting older
- Family history of bladder cancer
- Birth defects in the bladder or urinary tract
Other risk factors include:
- Smoking
- Exposure to chemicals at work or in the environment
- Bladder irritation caused by:
- Kidney and bladder stones
- Inflammation and infections
- Long-term catheter use
- Having had radiation to treat another type of cancer
Signs and Symptoms
Some common symptoms of bladder cancer include:
- Blood in your urine
- Pain when you urinate
- Having to urinate more often than usual
However, these symptoms can also be signs of bladder problems that aren’t cancerous. If you have these symptoms, make sure to see your doctor.
Understanding Your Cancer
Quick Guide to Coping with Bladder Cancer
Learn about coping with treatment side effects, tips for living with bladder cancer, and coping for caregivers. The video will also go over the stigmas behind having bladder cancer, palliative care, advanced care planning, and managing the cost of…
Diagnosis and Staging
Diagnosis
The process of finding out if you have bladder cancer and learning as much as possible about it is called diagnosis and staging. A complete diagnosis usually takes more than one doctor’s visit. It may involve scans, blood tests, and a biopsy. Your doctor will work with a team to figure out if you have cancer. They will also determine the type and subtype, and if and where it has spread.
Your health care team will want a detailed medical history if they suspect bladder cancer. They will then run tests to learn as much as they can about your bladder cancer. This process may include:
Physical exam – The exam will include questions about your medical history and any symptoms you may be experiencing.
Imaging (scans) – Scans provide a picture of the bladder and other areas. They are used to look for tumors or abnormal cells. They help determine the extent or spread of the cancer.
Blood work – Your care team may send blood samples to a lab to check blood counts and kidney function.
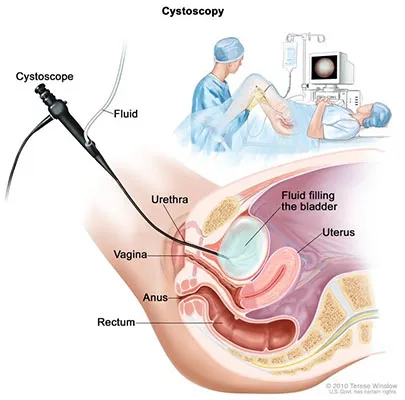
Cystoscopy Procedure – Your doctor may also send you to a urologist for a cystoscopy (sis-TOS-kuh-pee). This procedure allows your doctor to see and examine the inside of your bladder. During the procedure:
- Your doctor will insert a scope into your urethra, the tube that carries urine out of your body. The scope has a special lens that allows your doctor to get a close look at the lining of your bladder.
- Your doctor will fill your bladder with a sterile solution.
- Your doctor will remove a small piece of bladder tissue. This is called a biopsy. The tissue is sent to a pathologist, who will examine it under a microscope to see if there are any cancer cells.
From the biopsy, more information is gathered to determine the best treatment. This includes the type, grade, and stage of bladder cancer.
For more details about cystoscopy procedures, watch the video Having a Cystoscopy from our friends at Cancer Research UK.
Type
The results of the biopsy will help your doctor know what type of bladder cancer you have. This tells you and your healthcare team where the cancer started:
- Urothelial (transitional cell) – most common bladder cancer that starts in the cells that line the bladder and urethra
- Squamous cell carcinoma
- Adenocarcinoma
Grade
The grade describes what the cancer cells look like when viewed by a pathologist:
Low grade: less likely to come back
High grade: more likely to come back
Staging
The stage of the bladder cancer tells you and your health care team how far the cancer has spread. Bladder cancer can be non muscle invasive (Stages 0-1) or muscle invasive (Stages 2-4).
Non-muscle Invasive Bladder Cancer
When the tumor(s) have not spread into the bladder muscle. It is the most common form of bladder cancer. Three out of 4 patients diagnosed with bladder cancer have non-muscle invasive cancer. These tumors are Stage 0 (which can be further divided into stage 0a and stage 0is/Tis) or Stage 1 bladder cancer.
Also called Stage Ta or papillary tumors, these tumors are commonly found on a small area of tissue. Like other bladder cancers, it often returns, but it has a lower risk of spreading to the muscle after treatment.
Also called carcinoma in situ or CIS, is found on or near the surface of the bladder. It has a higher risk of of coming back after treatment.
Also called a T1 tumor, has spread into the bladder’s connective tissue, but not into the muscle. These tumors have a high risk of coming back and spreading into the muscle.
Muscle-invasive Bladder Cancer
The tumor(s) have grown into the muscle of the bladder and may have spread outside the bladder. About 1 out of every 4 bladder cancers are muscle-invasive. These tumors are Stage II (2), Stage III (3), or Stage IV (4).
The cancer has spread into the bladder muscle.
The cancer has spread through the muscle of the bladder to the fatty layer and/or has spread outside the bladder to nearby lymph nodes or tissue.
Also known as metastatic bladder cancer, has spread to the lining of the walls of the abdomen or pelvis. It may also have spread to other parts of the body.
Treatment
Key members of a treatment team for bladder cancer can include:
- urologist
- urology nurses
- wound/ostomy nurse
- medical oncologist
- oncology nurse
- radiologist
- palliative care specialist
- dietician
- social worker
- financial counselor
Learning about your treatment options will help you and your health care team with shared decision-making. Treatment for bladder cancer may involve a combination of treatments. And your treatment will be based on whether you have non-muscle invasive or muscle-invasive bladder cancer. Talk to your doctor about the risks and benefits of each type of treatment to determine which is best for you.
Types of Treatment
Surgery is an important part of both non-muscle invasive and muscle-invasive bladder cancer. As with other types of surgery, side effects include pain or discomfort, risk of infection, and some mobility restrictions right after surgery.
There are 2 main types of surgery:
- TransUrethral Resection of Bladder Tumor (TURBT) procedure – This surgery is the most common way to remove early-stage tumors.
- Partial or Radical Cystectomy – In this operation, part or all of the bladder and surrounding tissue are removed. The surgeon will also reconstruct the bladder. Learn more about bladder reconstruction.
The use of drugs to destroy or damage cancer cells so they cannot divide and multiply.
Treatment that uses the body’s natural defenses (immune system) to identify, attack, and kill cancer cells.
High-powered energy is used to shrink tumors, relieve pain and pressure, decrease symptoms, and improve quality of life.
Targeted therapy is a form of cancer treatment that may be used to treat bladder cancer. Targeted therapies block the action of certain genes, proteins, or molecules that cause cancer to grow and spread. Your doctor will need to test your tumor for biomarkers to find out if targeted therapy is right for you.
Medical care focused on relieving the symptoms and stress of a serious illness. It does not treat the cancer itself. It can be used at any age and at any stage. Palliative care is different from end-of-life treatment or hospice care. You can get palliative care while you are getting treatment for your cancer. The goal is to improve quality of life for both the patient and the family.
Palliative care is provided by a specially trained team of doctors, nurses, and other specialists. They work with your other doctors to provide an extra layer of support.
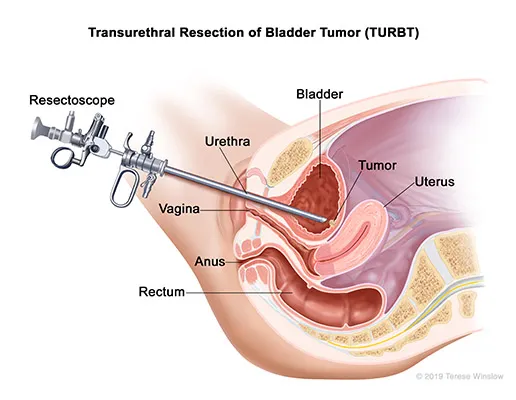
TURBT Procedure
If you have bladder cancer, your urologist will perform a surgical procedure called a transurethral resection of bladder tumor (TURBT). This is the most common way to remove early-stage tumors. For the procedure:
- You will be given anesthesia.
- Your urologist will insert a scope through the urethra into the bladder. This part is very similar to a cystoscopy.
- Your urologist will remove any abnormal looking tissue using the scope’s wire loop.
- A pathologist will look at this tissue under a microscope to learn more about the abnormal tissue.
What Is Maintenance Therapy for Bladder Cancer?
Ruby, your virtual community navigator, will help you understand what maintenance therapy is and how it can be used to treat bladder cancer.
Survivorship and Coping
A Healthy Lifestyle
Be sure to talk to your healthcare team about exercise, diet, and nutritional supplements. It is not yet known if these can help reduce the risk of your cancer returning or spreading. Eating a good diet, not smoking, being active, and staying at a healthy weight are good for your heart and overall health.
Scanxiety
Having to go for repeat testing or needing repeat surgeries can cause anxiety, sadness, depression, or frustration. These follow-up tests can also cause a great deal of stress. Follow-up cystoscopies may cause pain and discomfort, which can cause even more anxiety. Patients have nicknamed these feelings scanxiety.
Emotional Support
Whether you have cancer or someone close to you has cancer, it can be very helpful to talk with others in a similar situation who will understand what you are going through. Support from others who understand can help improve your ability to cope and feel more in control over your situation. It can also give you a sense of hope.

Diet & Nutrition for Cancer Survivors
People often finish cancer treatment and wonder, “Now what?” Here are some tips to lead a healthy lifestyle after cancer.
Survivorship
Cancer survivorship doesn’t begin when treatment ends. It starts at the time of your diagnosis. You can think of survivorship as having 2 parts:
From diagnosis through the end of treatment
During this time, your focus will be on learning more about the type of bladder cancer you have, your treatment options, and making treatment decisions that are right for you. Survivorship will also be about learning the best way to manage and cope with short-term symptoms or side effects that you have from your cancer or its treatments.
After treatment ends
During this time, your focus will be on adjusting to life after your initial treatment is over. At this time, your focus will be on understanding when you need to see your doctor for follow-up visits, managing any long-term side effects of your cancer and its treatments, and — for many patients — learning how your new bladder works.
The Bladder Cancer Advocacy Network (BCAN) provides support through their Survivor to Survivor program. The program provides support and information on coping with side effects to women and men at all stages of survivorship.
Survivorship Care Planning
A survivorship care plan is a document that includes information about the treatments you have received and the follow-up care you need. Having a survivorship care plan can help you keep track of all the treatments you’ve had, your test results, and when to follow up with your cancer care team. It can also help you keep copies of all medical records and insurance payments in one place. Because some types of bladder cancer have a high risk of coming back, these follow-up tests are very important.
You will also want to:
- Know what symptoms might suggest your bladder cancer has returned or spread so you can tell your health care team about them as soon as possible.
- Talk to your care team about your risk for other types of cancers.
- Talk to your care team about exercise, diet, and nutritional supplements. It is not known if they can reduce the risk of a recurrence. But we do know that eating a good diet, not smoking, being active, and staying at a healthy weight are good for your heart and overall health.
- Keep copies of all your medical records and insurance payments.
Read Liz's Survivorship StoryDo your own research. Ask the tough questions. Educate yourself about your conditions. Be aware of what potentially lies ahead so that you are better prepared to deal with it.
Caregiver Support
Bladder cancer affects not only those with the disease, but also the people who care for them. Caregiving for a person with bladder cancer can be stressful. You may feel angry, guilty, alone, afraid, or sad. If you are caring for a person with bladder cancer:
- Find support. Share your feelings with others. Look for caregiver support groups, either in person or online. Ask the patient’s cancer center if they have a support program for caregivers.
- Look for extra help. Ask family, friends, and members of your community if they can help. If they offer, give them specific tasks. If you can afford it, consider hiring people to help care for the person with bladder cancer. Or have them help with chores, childcare, or errands.
- Take breaks. Carve out time for yourself. Spend time with people important to you and take time for activities you enjoy. Don’t feel guilty about making time for yourself. It is important for your own health.
- Take care of yourself. Just as the person with bladder cancer needs to pay attention to their diet, exercise, and sleep, so do you. Be mindful of habits that may affect your overall health such as smoking or consuming alcohol.
- Learn about the Family and Medical Leave Act (FMLA). You may qualify to take up to 12 weeks of unpaid, job-protected leave to care for a seriously ill family member.
- Learn about financial assistance. You may have high out-of-pocket costs from parking, transportation, and food as part of your caregiving duties. Ask your care team if financial counseling is available. Discover tips to manage the costs of cancer treatment.
Frankly Speaking About Cancer Library
LibraryWould you like a print copy of these educational materials?
We can mail our Frankly Speaking About Cancer pieces to you. Shipping is free for up to 20 pounds.


