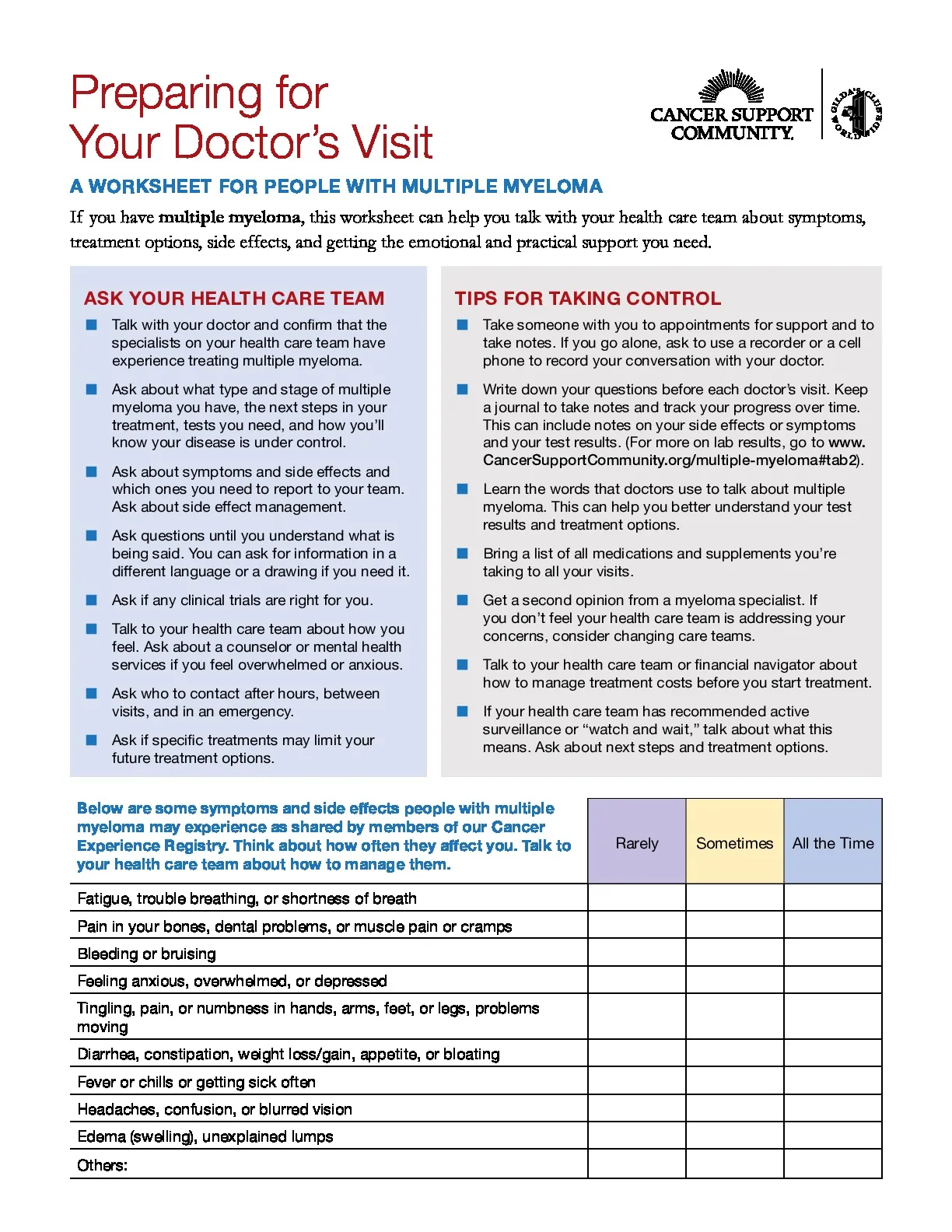
Multiple Myeloma
Table of Contents
Multiple myeloma (MM) is a blood cancer that starts in the plasma cells of bone marrow. This is the spongy material in the center of bones. The marrow makes stem cells. They mature into red blood cells, white blood cells, and platelets. Myeloma cells are abnormal platelets. With Multiple myeloma, the abnormal cells crowd out healthy cells, and cause many problems:
- Bone pain and fractures
- Anemia (low red blood cell count)
- Uncontrolled infections
- Kidney damage
Risk Factors
The cause for multiple myeloma is unclear, but the risks for getting multiple myeloma include:
- Age: Most patients are age 60 or older
- Gender: Occurs more among men than women
- Race: African Americans are twice as likely to get MM
- Weight: Being obese or overweight
- Genetics: People with a family history of multiple myeloma (hereditary or genetic connection)
- Medical conditions: People with MGUS or Monoclonal Gammopathy of Undetermined Significance. MGUS is when abnormal M proteins are present, but not enough to be diagnosed as “blood cancer.” 1 in 100 people with MGUS can develop blood cancer.
Symptoms
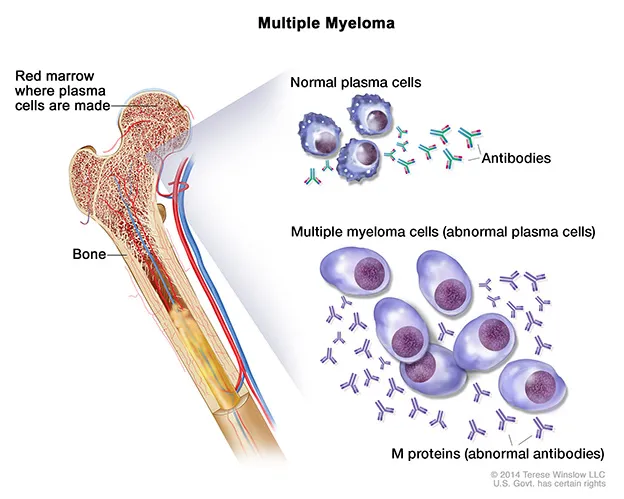
Multiple myeloma symptoms depend on the stage of your disease and your body’s response. Symptoms for multiple myeloma are known as “CRAB” symptoms. These include: high levels of calcium, renal (kidney) problems, anemia, and bone problems.
What Is Multiple Myeloma?
This video will help you understand what multiple myeloma is, as well as its symptoms and treatment options. Have a concern of your own? Please call our Cancer Support Helpline to talk with an experienced counselor or navigator: 888-793…
Diagnosis and Staging
Your doctor will talk with you about your health. They’ll order different kinds of blood tests if they suspect a blood cancer. They might also run urine tests, scans, a bone marrow biopsy, and biomarker tests on your bone marrow. Your test results will help determine the best treatment plan for you.
- The complete blood count (CBC) counts the number and types of blood cells in a blood sample. Learn more about complete blood counts and normal results.
- The serum protein electrophoresis (SPEP) finds and measure M proteins.
- Immunofixation or immunoelectrophoresis finds the exact type of abnormal M protein antibody.
- A blood calcium tests the level of calcium in your blood (a sign of bone loss)
- Beta 2-microglobulin (ß2M) level tests how much ß2M is in your blood or urine.
- The serum free light chain (SFLC) assay test looks for excess amounts of proteins called light chains.
- 24-hour urine test looks for the Bence Jones protein (parts of M protein) and other abnormal immunoglobulins (signs of kidney damage).
- Chemistry profile tests, also called metabolic panel tests, measure how well the kidneys and liver are functioning.
Such as a skeletal survey, x-rays, MRI, CT, or a PET scan, to look for bone damage and lytic lesions (spots where bone tissue damaged) caused by multiple myeloma.
- Looks at the cells in bone marrow.
- It confirms if cancer cells are present, and what type.
Biomarker tests look for changes in the DNA of cells. Types of tests include:
- Fluorescence in situ hybridization (FISH)
- Immunohistochemistry and Flow cytometry
- Cytogenetics and Karyotyping
- DNA Sequencing
Staging & Types
Myeloma is diagnosed from Stage 1 (least aggressive) to Stage 3 (most aggressive). It is diagnosed as:
- Asymptomatic (smoldering) myeloma: when the M protein levels are high, and urine tests results are abnormal, but there are no “CRAB” symptoms. If this is the case, you may only need active surveillance to watch for any changes.
- Symptomatic (active) myeloma: when M protein levels are high and the bone marrow biopsy contains plasma cells, but one or more “CRAB” symptoms are also present. Once myeloma becomes active, it will remain active. Treatment is recommended.
- Sometimes plasmacytoma is found in scans. This means that only one mass of abnormal myeloma cells are seen (rather than “multiple”).
Your M Protein Level
It’s important to learn what your M protein level is, and track changes over time. This is the main biomarker that tells you if MM is advancing.
If the M protein level is…
- Less than 3 g/dL – You may have MGUS, with a 1% risk per year for MM or related conditions.
- Greater than or equal to 3 g/dL – You may have asymptomatic myeloma, with a 10% risk per year for active myeloma.
- Greater than or equal to 3 g/dL plus at least one “CRAB” issue (high calcium, renal problems, anemia, bone problems) – You may have active myeloma.
What Does the African American Community Need to Know About Multiple Myeloma?
Ruby, your virtual community navigator, will help explain what members of the Black and African American community needs to know about multiple myeloma, the second most common blood cancer in the United States.
Treatments and Side Effects
A hematologic-oncologist (HEE-muh-tuh-LAH-jik on-KAH-loh-jist) is the doctor trained to treat blood cancers. Try to find one who treats many multiple myeloma patients and knows a lot about new treatments. There are many treatments available to manage multiple myeloma. New research in clinical trials is looking for a cure.
There are a number of treatments that work to manage multiple myeloma. Until a cure is found, multiple myeloma is managed like a chronic illness. Some people can live for years without treatment. Most people will need treatment on and off throughout their life.
Treatment Planning
It’s important to think about the steps you can take and talk with your doctor about what you want to do. This is called treatment planning.
Treatment decisions are based on:
- The results of biomarker tests and the stage of your multiple myeloma
- Your values, goals, and preferences
- Your age
- Your health and symptoms (including whether you have kidney disease, heart disease, anemia, or other illnesses)
- Your medical history and what treatments you’ve had for multiple myeloma
Questions to ask your healthcare team include:
- Which treatment(s) do you recommend? What is the goal of the treatment?
- When will treatment start? When will it end? How often and where will I have my treatment?
- Do you recommend a stem cell transplant? If so, what should I do to prepare? How will I feel during and after this treatment?
- Do I need a caregiver during and after treatment? If so, for how long?
- What can I do to feel better during recovery?
- What side effects should I anticipate? Can I prevent or treat any of these side effects?
- Will there be long-lasting side effects? What can I do about them?
- How will I know if my treatment is working?
- How often will I need checkups? What follow-up testing will I need and how often?
- What information do you have so I can learn more about this treatment?
- What types of resources are available to me during my treatment (i.e. social worker, nutritionist, case manager, financial resources)?
- Who will be a part of my health care team and what is the role of each member?
- What stage is my disease? What does this mean in regards to my treatment?
- Is my kidney function being affected?
- How will the recommended treatment affect my life on a daily basis? Will I be able to continue with my normal activities as I do them now?
- (If applicable) Could this treatment affect my fertility? Would you recommend I consult with a fertility specialist before beginning treatment?
- Should I seek a second opinion prior to beginning treatment? If so, who would you recommend I see?
- Are there clinical trials open to me? How do I find out more about these trials?
Treatment for Symptomatic Multiple Myeloma
Welcome to the Quick Guide to Treatment for Symptomatic Multiple Myeloma. This Quick Guide will cover different treatment options for Symptomatic Multiple Myeloma. We will also give a brief overview of symptoms and side effects. Learn More About…
Treatment for Asymptomatic (Smoldering) Multiple Myeloma
Active Surveillance (regular testing only) can be used for many years. It is used when cancer is growing slowly and not causing symptoms. Healthy exercise and diet habits always help, and may slow progression. Get more details about active surveillance and tips on how to cope.
Treatment for Symptomatic (Active) Multiple Myeloma
The choice of treatment(s) you start with depends on the current stage of your disease. It also depends on how far it has progressed and your overall health. Most treatments for multiple myeloma use more than one drug at one time. Different combinations are used at different times in a patient’s life.
Review your treatment options:
- Chemotherapy
- Targeted Therapy
- Hormone Therapy
- Immunotherapy
- Stem Cell Transplant
- Supportive Care Drugs
Chemotherapy (also called chemo) uses drugs to destroy or damage fast-growing cells like cancer cells. It is used to shrink tumors, slow cancer’s growth, relieve symptoms, or help people live longer.
Targeted therapy drugs are used to block the growth of myeloma cells by blocking the action of abnormal protein that stimulates the growth of myeloma cells. These drugs are more targeted than traditional chemotherapy, but they may still cause side effects that can include nausea, gastrointestinal problems, and possibly nerve damage and numbness.
Steroids, in high doses, are used to trigger the death of myeloma cells. They also help decrease side effects like nausea and vomiting from chemotherapy. Some steroids are used to treat inflammation.
Immunotherapy is a type of cancer treatment that uses the body’s natural defenses (the immune system) to identify, attack, and kill cancer cells.
A stem cell transplant can lead to a long cancer remission. For multiple myeloma patients, it can be done more than once (after relapse). A stem cell transplant is an infusion of blood-forming cells (stem cells), not a surgery. It allows your health care team to use higher-dose chemotherapy to kill multiple myeloma cells than would otherwise be safe. An autologous or "auto" stem cell transplant which uses your own stem cells, is most often used for multiple myeloma.
Growth factors treat myeloma by helping the bone marrow produce more blood cells. They are used to increase low blood counts with growth hormones and colony stimulating factors.
Treatment for Relapsed and Refractory Multiple Myeloma
Treatment for Relapsed MM
When cancer returns after treatment, more treatment is offered. Different drug combinations may be tried. A clinical trial may also be an option.
The treatment offered after relapse depends on:
- Disease-related symptoms
- The risk of another relapse
- Your general health
- Past treatments
- How well past treatments worked
Treatment for Refractory MM
When cancer doesn’t respond to treatment, your doctor may offer another type to try. Or, a clinical trial may be an option. Supportive care and palliative care are available to help with pain and discomfort.
Clinical Trials
Be sure to ask about clinical trials. These are studies to test new treatments or learn how to use current treatments better. They may be the only way to try a promising new treatment. There are several new things being tested for multiple myeloma. Trials are often recommended for refractory disease (when other treatments don’t work).
Aredia Taylor: We Don't Have to Suffer in Silence
Managing Symptoms & Side Effects
Common problems from multiple myeloma include:
- Pain – Can be the cause of the myeloma itself, or from a biopsy, or treatment.
- Bone pain and weakness – Myeloma cells can weaken and damage bones. Your health care team may make diet or exercise recommendations to help with this problem. When diet and exercise are not enough, bone strengthening drugs, radiation, orthopedic supports, or surgery can help.
- Anemia – When your red blood cells don’t carry enough oxygen through your body. This can make you feel tired and weak, out of breath, or dizzy.
- Infections – When your white blood counts are high, your risk for infections is high. Even a small infection can be serious. Get help immediately if you have an infection.
- Kidney problems – The kidneys help clean the blood to remove waste (urine) and keep water balance. Some people with MM develop kidney problems from the disease and/or its treatment. Talk about strategies to protect your kidneys with your doctor. Get tips on how to care for your kidneys.
Supportive care is used to manage symptoms at any stage of the disease. Eating well and doing daily exercise will also help with symptoms and side effects.
Make sure to let your health care team know if you experience any of these symptoms.
Coping and Support
Multiple myeloma is unique because it often has to be managed over a lifetime. There are periods of remission (when the cancer goes away) to periods of relapse (when the cancer returns). Managing the stress and anxiety of life with MM can be difficult. It’s hard to be unsure of what the future holds.
You can regain control by taking an active role in the way you approach your life and care. If you feel depressed, it’s very important to seek help right away.
Tips for Coping
- Ask your health care team questions until you understand your diagnosis and why they recommend a certain treatment plan.
- Know if there are signs or symptoms that you should report right away.
- Keep a notebook to track questions, how you feel, and information you learn. Bring this with you to appointments.
- Learn as much as you can and talk with other experts. Get a second or third opinion at any stage of your care. You are in control of your choices and can make changes along the way.
- Control what you can. If you smoke, get help to stop. Exercise regularly, as long as it is approved by your care team. Eat healthy foods and maintain a healthy weight.
- Know that you will be more anxious when it gets close to your doctor’s appointments. Learn relaxation techniques (like deep breathing and meditation). Be gentle with yourself.
- Get the help you need if you feel anxious or stressed. Your medical team can refer you to a support group, one-on-one counseling, organizations that specialize in multiple myeloma, or connect you with another patient who’s ‘been there’ and may be a friend.
- Find resources for support in our Frankly Speaking About Cancer: Multiple Myeloma book.
- Consider your priorities and ask yourself: how can I gain meaning in my life? Can I do things that give me a sense of peace or belonging? Can I spend time doing things that I enjoy and are important to me?
Caregiver Support
Multiple myeloma affects not only those with the disease, but also the people who care for them. Caregiving for a person with multiple myeloma can be stressful and frustrating.
If you are caring for a person with multiple myeloma, here are some tips:
- Find support.
- Look for extra help.
- Take breaks.
- Take care of yourself.
- Learn about the Family and Medical Leave Act (FMLA).
- Learn about financial assistance.
Share your feelings with others. Look for caregiver support groups, either in person or online. Ask the patient’s cancer center if they have a support program for caregivers.
Ask family, friends and members of your community if they can help. If they offer, ask for help with specific tasks. If you can afford it, consider hiring people to help with caregiving. Or have them help you with chores, childcare or errands.
Carve out time for yourself. Spend time with people important to you, and take time for activities you enjoy. Don’t feel guilty about making time for yourself. It is important for your own health.
Just as a person with MM needs to pay attention to their diet, exercise and sleep, so do you. If you smoke, find a smoking cessation program. Limit alcohol.
You may qualify to take up to 12 weeks of unpaid, job-protected leave to care for a seriously ill family member.
You may have to deal with costs from parking, transportation and food as part of your caregiving duties. Ask the hospital if they can provide financial counseling, or even stipends, for caregivers.

Coping With Multiple Myeloma
We talk with Dr. Sikander Ailawadhi and Jan Miller, a licensed professional counselor, about the knowledge and tools that can help manage the impact of living with multiple myeloma.
Costs and Expenses
Treatment for multiple myeloma and follow-up care can be costly, and overwhelming. Many families say that financial worries about cancer costs are a big source of stress. It’s hard to know where to turn.
Frankly Speaking About Cancer Library
LibraryWould you like a print copy of these educational materials?
We can mail our Frankly Speaking About Cancer pieces to you. Shipping is free for up to 20 pounds.
Your Experience Matters
Help improve outcomes for multiple myeloma patients & caregivers. Join the Cancer Experience Registry.