Breast Reconstruction
What Is Breast Reconstruction?
Breast reconstruction is surgery that is done to rebuild the shape & look of the breast after treatment for breast cancer. Most people with breast cancer will have some type of surgery as part of their treatment.
There are different types of surgeries to treat breast cancer. The goal of the surgery may differ depending on the location of the cancer and stage:
- Breast-conserving surgery removes the cancer and some of the surrounding tissue. It is also known as a lumpectomy, quadrantectomy, partial mastectomy, or segmental mastectomy. During this procedure, only part of the breast and tissue is removed. How much breast tissue is removed will depend on the location and size of the tumor.
- A mastectomy is a type of surgery that removes the entire breast. All of the breast tissue and sometimes the lymph nodes are removed. Some people may have both breasts removed as a form of treatment. This is called a double mastectomy. Typically, most of the skin of the breast can be saved. Sometimes the nipple can be saved as well. This is called a nipple-sparing mastectomy.
Breast Reconstruction - Knowing Your Rights As A Patient
Immediate vs. Delayed Breast Reconstruction
Your doctor may suggest either immediate reconstruction or delayed breast reconstruction surgery. They will base this suggestion on your health, your treatment needs, and the type of tumor you have.
Immediate Reconstruction
Immediate reconstruction occurs at the same time as the mastectomy or breast-conserving surgery. Most of the time this is completed in stages, and you may need at least two operations.
There are several advantages to immediate breast reconstruction. For example, you may have more chest tissue to support the procedure at the time. This is because there is no surgical scarring or changes caused by later cancer treatments. Starting breast reconstruction at the same time as the mastectomy also means less surgery and exposure to general anesthesia overall. You can also recover from everything at the same time. With this, physical changes after a mastectomy may not be as dramatic.
Delayed Reconstruction
Delayed reconstruction can give you more time to adapt emotionally and research your reconstruction options. Some people prefer to have more time to recover from their mastectomy before beginning reconstruction. You may still have the option to undergo reconstruction surgery later on.
In some cases, your doctor may ask you to wait to have reconstruction surgery. People who have diabetes or have a higher weight are often asked to wait to avoid surgical risks. This is often the case for people who smoke as well. If you currently smoke, your surgeon may require you to stop before moving forward with the surgery.
If radiation therapy is or was part of your cancer treatment plan, ask your doctor about the best timing for the procedure. Radiation reduces the elasticity of skin tissue and can change how well blood travels to the area. This can impact the reconstruction procedure. Talking with your doctor about timing can help reduce any damage to the reconstructed breast.
I had no idea that breast reconstruction for symmetry is a law. I sure didn’t expect to be happy about breast cancer, but to learn that laws have acknowledged this super important part — that’s definitely an unexpected gift.
Is Reconstruction Right for Me?
Choosing to undergo breast reconstruction is a very personal decision. You can choose not to have the additional surgery as well. It is important to acknowledge your feelings along with any fears you have. Operating from a place of clarity will enable you to make informed, timely decisions throughout your cancer experience.
Take a moment to prioritize what is important to you when considering your breasts after cancer. How you felt about your breasts before cancer, your treatment plan, and other considerations can influence how you wish to deal with reconstruction surgery. Think about how you feel about your breasts as part of your self-image. How will breast surgery affect your life? Remember this is still YOUR body and YOUR decision. Determine what you feel most comfortable with.
There are alternatives for people who decide not to have reconstruction surgery. These include choosing to go flat or using a breast form. If you decide that you do not want to replace the removed breast(s), you can choose to go flat. This option rarely causes issues for people who have had both breasts removed. For those who only have one breast removed, there may be some issues with posture, balancing, and back pain. This is especially the case for people with larger breasts. To help, a breast form may be a better option.
A breast form is a type of prosthesis, or artificial body part. It can be worn inside a bra or attached to the body. It can help with balance and mirror the look and feel of a natural breast under clothes. There are many cancer centers and local shops that specialize in providing these supplies for people with breast cancer.
Think About Who You Are And Where You Are In Life
Types of Breast Reconstruction Surgeries
The two main types of breast reconstruction surgeries are implant reconstruction and reconstruction with a tissue flap. You may be able to have a procedure that combines both. With this option, your surgeon may use a breast implant along with tissue from your own body.
Here is a further look at these different types of reconstruction surgeries:
Implant Reconstruction
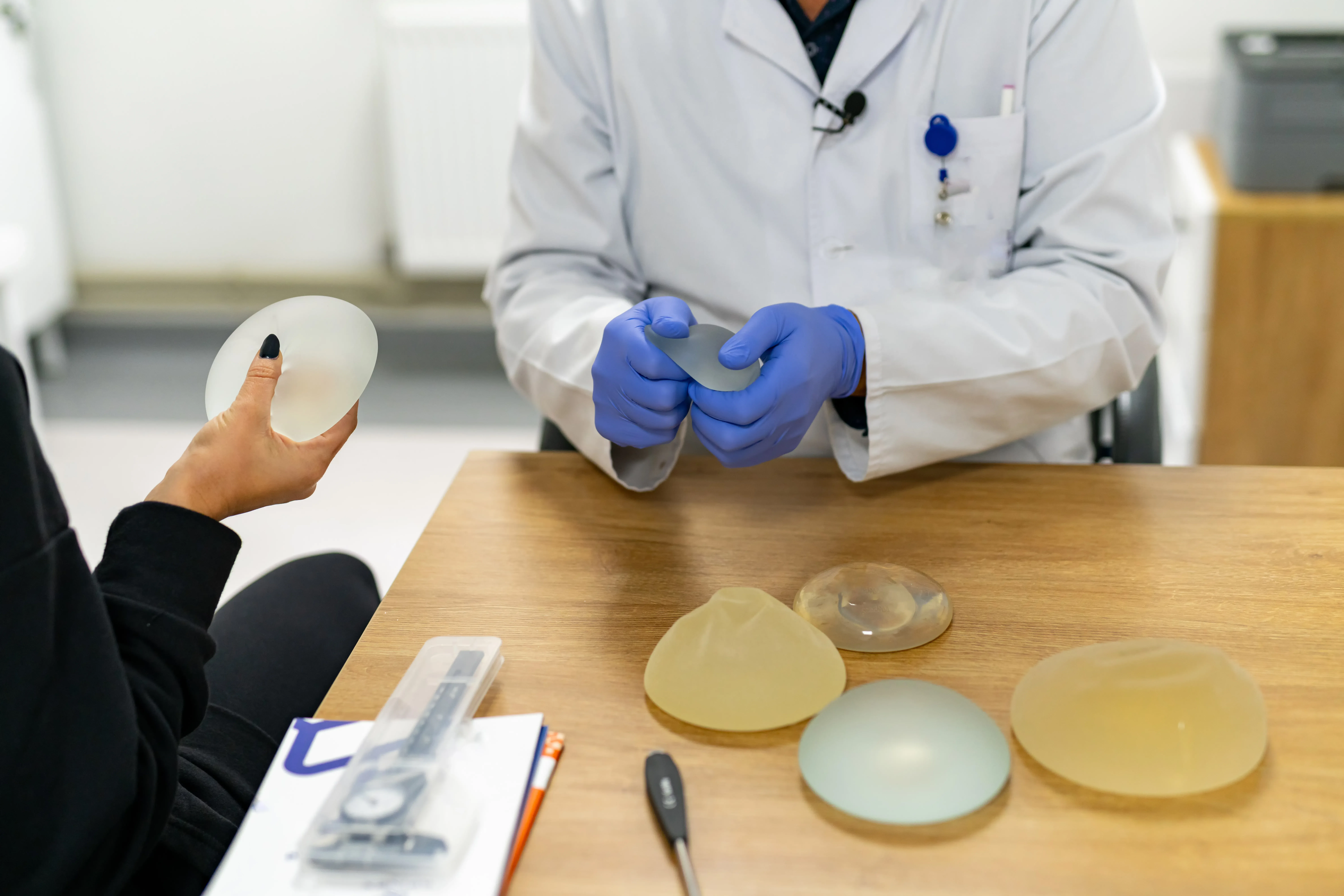
Implant reconstruction involves the use of a breast implant. The implant helps restore the shape of the removed breast. There are two common types of implants: a saline implant and a silicone-gel filled implant. Both types are approved for use during breast reconstruction by the FDA (U.S. Food & Drug Administration).
A saline implant has a silicone outer shell. It is filled with a sterile saline solution. The saline solution is like salt water. The silicone-gel filled implant has a silicone outer shell as well. Instead, it is filled with a type of silicone gel. Both types of implants can come in different sizes. They can come in a smooth or textured outer shell. Ask your surgeon if you can feel a sample of each type. It may be helpful to talk with others who have had these implants to help with your decision.
Implant reconstruction is typically performed in stages after a mastectomy. It may involve at least two surgical operations:
- During the first stage, your surgeon will place a tissue expander under the skin or muscle on your chest. The tissue expander is like a water balloon. When the expander is placed under your skin, it is flat. A saline solution is inserted into the expander at the time of the mastectomy, through a small valve. During later doctor visits, more saline is added to help stretch the breast area. This occurs until the tissue expander reaches the desired size. Some people mention that the expander feels tight or “like rocks” while in place. Sometimes the tissue expander is held in place with mesh, like a sling.
- During the second stage, the tissue expander is removed. Your surgeon will replace it with a permanent breast implant. The second stage can be planned further in advance or postponed if needed. Additional surgery stages may take place if needed. Additional surgery can help improve the overall look of the implant or recreate the nipple-areola.
Very few people are able to have breast implant reconstruction performed in one stage. When this occurs, the breast implant is put directly in place at the same time as the mastectomy. This is called direct to implant breast reconstruction. This procedure is typically available to people who have smaller breasts, are younger in age, and have no immediate health concerns.
During a direct to implant reconstruction, a tissue expander is not used. Once the breast tissue is removed, a plastic surgeon places the implant under the skin or muscle on the chest. Additional surgery may be needed to improve the overall look of the breast or for nipple reconstruction.
What You Should Know About Implants
Concerns About Implants
The U.S. Food and Drug Administration (FDA) has determined that most saline and silicone filled implants are safe for breast reconstruction. Discuss any concerns you have about implants with your doctor. Also, your doctor should explain to you that any implant—whether it is made from saline or silicone—may need to be replaced with surgery at some point in your lifetime. That’s because implants can leak or tear over time, which may lead to infection. Implants can also develop scar tissue. These risks can be managed effectively by your surgeon and with proper care. Talk with your surgeon about any concerns you have with implant reconstruction.
More on breast implant safety is available at:
Tissue Flap Reconstruction
A tissue flap procedure uses tissue from your body to rebuild the breast. The tissue may be removed from your abdomen, back, thighs, or buttocks. This procedure is also called an autologous reconstruction.
Tissue flaps tend to look and feel more natural. They also behave more like natural breasts than implants. For example, tissue flaps will shrink or expand when you lose or gain weight. Unlike some implants, tissue flaps will not need to be replaced during your lifetime. In some cases, tissue flaps are used with a breast implant to create more volume in the breast.
Tissue flap reconstructions typically involve more surgery than implant reconstruction. This procedure also has a longer recovery period. Tissue flap surgery will result in two scars. One scar will form at the breast surgery site. The other scar will form in the area where tissue was removed. These scars may fade over time but will never go away completely.
Some people may also run into challenges in the area where the tissue was taken. This can include muscle damage or weakness or distortions in the skin, like dimpling. When tissue is removed from the abdomen, other changes may occur. For example, the shape of your belly button may change. The abdomen may also require extra support as it heals after the procedure. This helps to reduce other problems such as hernias or bulges. Be sure to talk with your treatment team about any questions or concerns you may have.
Tissue Rearrangement
If you have breast-conserving surgery, your surgeon may perform tissue rearrangement. During this process, your surgeon will take any remaining breast tissue and reform it into the desired shape and size. This procedure is typically for people with large breasts who want to decrease in size.
Once the lumpectomy is complete and the cancer is removed, a plastic surgeon will rearrange the remaining tissue to reform the breast. They will also perform a symmetry procedure on the other unaffected breast. This is usually a size reduction (mastopexy) and/or a procedure to lift the breast. Radiation therapy can be performed after this type of reconstruction.
Nipple and Areola Reconstruction
Nipple and areola reconstruction is usually the final step in breast reconstruction. Tissue from other areas in the body can be used to recreate the new nipple. It can be taken from the reconstructed breast, opposite nipple, abdomen, or buttocks for example. Newer methods, such as three-dimensional tattooing, may also be available with local experts. Tattooing can give the nipple a natural color and create the areola region on the breast.
Reconstruction & Recovery
What to Expect from Reconstruction Surgery
Reconstruction surgery is performed in a hospital, at an ambulatory surgery center, or at an office-based surgical center. Some follow-up procedures may be performed in your plastic surgeon’s office. Depending on the type of breast reconstruction procedure you choose, you may be able to go home that same day. If not, your doctor will have you remain in the center for a few days.
During the procedure, you will be given medication to make sure you are comfortable. You may receive general anesthesia or intravenous (IV) sedation. With general anesthesia, you are in a deep sleep and will not feel any pain. IV sedation works in a similar way. You are given a pain-blocking drug through a needle in the vein and in the breast tissue. You may fall asleep or be awake during the procedure. But you won’t feel any pain and will not remember much about the surgery.
When you attend follow up procedures you may only need local anesthesia. Local anesthesia numbs specific areas of the body. This is used for more minor procedures. You will be awake during this time, but you won’t feel any pain in the area.
Side Effects & Risks
Like any major surgery, your surgeon should explain and discuss any side effects and concerns related to your procedure. Your surgeon should also talk with you about any methods to prevent future risks. Talk to your doctor about any questions or concerns you have.
Some immediate side effects and risks to be aware of, include:
- Bleeding
- Pain
- Fatigue (tiredness)
- Physical weakness
- Infection
- Blood clots
- Fluid build-up in the surgical area (seroma)
- Reactions to medications or anesthesia used during surgery
- Bruising and swelling
- Difficulty healing
Some side effects that can develop later, include:
- Excessive scar tissue
- Tissue death (necrosis)
- Loss of sensation in the breast or nipple
- Lymphedema (swelling due to fluid build-up)
- Changes in the arm on the same side as the reconstructed breast
- Breast implant problems (leakage, wrinkling, movement out of place)
- Scar tissue forms around the implant (capsular contracture)
- The need for extra surgery to fix any problems or improve breast appearance.
Soon after surgery, your ability to be physically active will change. Some exercises can help with recovery. Exercising can also help improve physical functioning over time. Ask your doctor about what exercises may be safe to do as you recover.
Physical Effects of Treatment
Breast cancer surgery can lead to some longer-term physical changes. You may experience chronic pain and even decreased strength or mobility. Some other physical side effects may include:
- Lymphedema: Lymphedema describes swelling in parts of the body caused by fluid buildup.
- Axillary web syndrome (AWS): AWS may occur if you have surgery that involves your lymph nodes. It is also known as ‘cording’. If you develop AWS, you may see and/or feel a web of thick, ropelike structures under the skin of your inner arm on the side of the operated breast.
- Phantom breast syndrome (PBS). PBS occurs when people feel sensations in the area where a breast was removed. This is usually caused by remaining pieces of breast tissue after surgery. These sensations can include pain and discomfort, itching, tingling, and even pressure in the area.
Talk to your doctor if you experience any of these or other new physical changes. They will be able to provide specific medications, therapies, and recommend lifestyle changes to help. Seeing a specialized physical therapist can also be helpful to prevent or treat symptoms like lymphedema and AWS.
Seeing a palliative care specialist can help address many side effects that may arise during treatment. Palliative care is different from hospice care and end-of-life care. It is available to you at any point of your treatment experience. Palliative care or supportive care can help you maintain your best possible quality of life. It can help you with physical, social, emotional, or spiritual concerns.
Long-Term Follow Up
You will need on-going follow-up visits with your surgeon after surgery. During this time, they will make sure you are recovering well and remove any surgical drains that may be in place.
A surgical drain is a small, thin tube. It is placed under your skin to help remove excess fluid or blood from the surgery site. Before you go home after surgery, make sure you understand how to care for any drains and incisions. Ask your doctor about bathing and showering.
During follow-up visits with your surgeon, they may discuss the next steps in your reconstruction journey. For people who have implant reconstruction, MRI scans may be recommended in some cases. This scan will allow your surgeon to check the condition of your implant and make sure it is still in place and is not leaking. You may need a scan every 1 to 2 years after the initial follow-up visit.
Recovery: It Took A Lot Longer Than I Expected
Survivorship & Recurrence
Many people who complete their treatment for cancer often fear that it will return (cancer recurrence). It is important to know that breast reconstruction does not cause breast cancer recurrence. Implant and tissue flap procedures do not disguise the cancer or hinder the ability to detect it.
After treatment, ask your doctor or oncology nurse for a ‘survivorship care plan’ specific to you. A survivorship care plan will:
- List out what follow-up care you’ll need over time
- Include any next steps for you and your care team to monitor your cancer
For example, your survivorship care plan may advise you to have regular mammograms on your breasts every year. In most cases, people who had a mastectomy may not need a mammogram on the reconstructed breast. If you have implant reconstruction surgery, your care plan may advise you to see your plastic or breast surgeon every year.
Coping with Breast Cancer and Reconstructive Surgery
It is important to take care of yourself as you navigate life after a breast cancer diagnosis. Managing both the emotional and physical impact of cancer can lead to a lot of stress.
It helps to have support, both during and after cancer treatment. Talking with people who understand your experience can help you cope and feel in control. There are many places to turn to for practical and emotional support, including:
- Health care facility: Your health care facility may be able to connect you to a patient or nurse navigator. These specialists can be a key resource during your treatment journey and recovery.
- Psychologist, therapist, or mental health counselor: These professionals are specially trained to support people and their emotional, behavioral, and social concerns.
- Spiritual/ Faith leader in the community: This person can provide religious or spiritual support.
- Support groups or peer mentors: Talking with others who have experienced similar stressors can help you better understand and express what you are feeling. Your care team may be able to recommend online or in-person support groups.
- Local or national patient advocacy groups: Look for groups that work with people diagnosed with breast cancer or people who had breast reconstruction surgery. They can provide a variety of support and resources throughout your experience.
Recovery: The Masectomy Was A Loss - The Reconstruction Was A Gain
Would you like a print copy of these educational materials?
We can mail our Frankly Speaking About Cancer pieces to you. Shipping is free for up to 20 pounds.

