What is Bone?
You probably don’t spend much time thinking about your bones, but there is a lot going on inside them. Bone is living growing tissue made up of proteins and minerals. Your bones have two layers. The outer layer, called cortical bone, is very thick. The inner layer—the trabecular (truh-BEH-kyoo-ler) bone—is very spongy. Inside the spongy bone is your bone marrow. It contains stem cells that can develop into white blood cells, red blood cells, or platelets.
How Healthy Bones are Made
The cells inside our bones are always changing. There are three types of cells that are only found in bone:
- Osteoclasts (OS-tee-oh-klasts), which break down the bone
- Osteoblasts (OS-tee-oh-blasts), which form new bone
- Osteocytes (OS-tee-oh-sites), the cells inside the bone (these cells start out as osteoblasts).
Your body’s hormones control how fast these cells work. Up until age 20, the osteoblasts work faster than the osteoclasts, and you build more bone than you break down. After that, the osteoclasts start working faster than the osteoblasts, and your body breaks down bone faster than it builds it. This causes your bones to thin.
Cancer and its treatments can also affect the bone-building process, causing your bones to thin more quickly. A healthy diet, exercise, preventing falls, and taking bone-building drugs (if you need them) can help keep your bones strong, reduce your risk of broken bones, and improve your wellbeing as a cancer survivor.
Click here to watch our Facebook Live with Dr. Dawson who talks more about bone health.
Other Resources If This Page Isn’t For You
For people with bone cancer:
- You can learn more about cancer that starts in the bone in our Bone Cancer web pages.
- You can learn more about cancer that starts in the bone marrow in our Multiple Myeloma pages.
For people with bone metastasis:
Cancer can spread to the bones from the breast, lung, prostate, or other organs. This is called “bone metastases” or “bone mets.” It is not the same as bone cancer. You can learn more about bone metastases in our Bone Metastasis pages and in our booklet “When Cancer Spreads to the Bone.”
Osteoporosis & Your Risk
What are Osteopenia & Osteoporosis?
As you get older, the tissue inside your bone changes. These changes make it easier for your bone to break if you fall or get injured. The medical terms for these changes are:
- Osteopenia (OS-tee-oh-PEE-nee-uh)—bone tissue is thinner than normal.
- Osteoporosis (OS-tee-oh-puh-ROH-sis)—bone tissue has become very thin and can break more easily.
Both are very common. About
- 43.4 million older adults have osteopenia.
- 10.2 million older adults have osteoporosis.
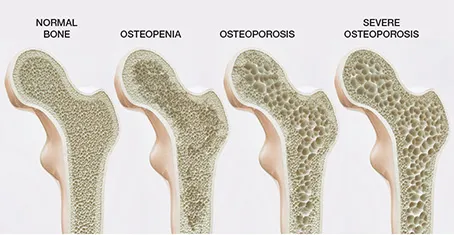
Osteoporosis means “porous” bone. Porous is a word used to describe something with small holes. These images show how as bones become thinner the holes become larger.
Risk Factors for Osteoporosis
Women start out with thinner bones and lose bone more rapidly than men do. This is why women are more likely than men to do develop osteoporosis. Other risk factors include:
- Being small and thin
- A family history of osteoporosis or hip fracture
- Height loss or stooped posture
- Going into menopause (the time in a woman’s life when her period stops) at age 45 or younger
- Breaking a bone after age 50
- Having rheumatoid arthritis
- Having a diet low in calcium and/or vitamin D
- Not getting enough physical activity
- Smoking
- Drinking too much alcohol
- Getting Specific kinds of cancer treatment (see below)
Bone Density Testing
The only way to know if you have osteopenia or osteoporosis is to have a bone mineral density test. The “density” is determined by the amount of calcium and other minerals that are inside your bones.
- Women usually have their first bone density test at age 65. But those who have a risk factor for osteoporosis (like a cancer diagnosis), may start earlier.
- Men usually have their first bone density test age 70. Men between age 50 to 69 who have been treated for cancer may also need a bone density test. It will depend on the treatments they received.
DEXA Scan Test
A DEXA can is the test most often used to measure bone density. The test uses low levels of X-rays to measure how much calcium and minerals are in the bones in your hip, wrist, and spine. The test is painless.
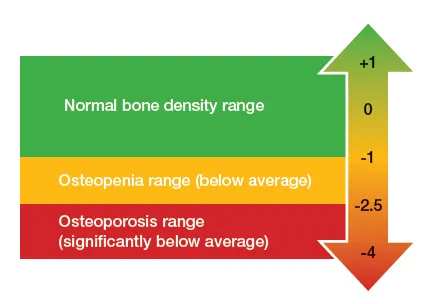
The results give your bone density a “score.” Here is what the score means:
- 0: bone mineral density is equal to that of a 30-year-old adult
- Between +1 and -1: bone mineral density is normal
- Between -1 and -2.5: bone mineral density is low (osteopenia)
- -2.5 or lower: bone mineral density is significantly low (osteoporosis)
Fracture Risk Assessment Tool (FRAX)
A FRAX score is an estimate of how likely you are to break a bone in the next 10 years. Your score is based on your:
- age
- weight
- gender
- smoking history
- alcohol use and
- whether you have had one or more broken bones in the past.
Your doctor will use your DEXA scan and FRAX scores to decide whether you should take a bone building drug.
Cancer Treatments that Increase Your Risk of Osteoporosis
Some cancer treatments can cause your bones to become thinner and break more easily. This type of bone loss occurs more rapidly and is more severe than bone loss that typically occurs in women and men as they age.
People with breast, ovarian, or prostate cancer are at highest risk for osteoporosis. They often get treatments that reduce the hormones that help their cancer grow. But the same hormones also control how fast the osteoblasts and osteoclasts work. Reducing the hormone levels slows the cells down, resulting in bone loss.
Women Who are Most at Risk
Certain cancer treatments increase risk for osteoporosis. The women most at risk have:
- Breast cancer treated with an aromatase inhibitor—anastrozole (Arimdex®), letrozole (Femara®) or exemestane (Aromasin®). If you are on an aromatase inhibitor, you should have bone density tests every two years, take calcium and vitamin D supplements, and talk to your doctor about whether to take a bone building drug.
- Breast cancer treated with tamoxifen (Nolvadex®) before they reach menopause. For these women, tamoxifen may slightly increase the risk of broken bones. In women who are menopausal, tamoxifen increases bone density.
- Cancer treatments that put them into early menopause. This can be chemotherapy, drugs that stop the ovaries from producing estrogen, or surgery to remove the ovaries.
Note to women with early-stage breast cancer: Your breast cancer treatment may include a bisphosphonate, typically zolendronate (Zometa®). It helps reduce your risk of having your cancer come back (recur) and spread to your bones. If your doctor suggests you take a bisphosphonate, be sure to ask whether the treatment is for osteoporosis or for your cancer. Treatments to prevent cancer from coming back are given more often (every six months) and for about 3 to 5 years.
Men Who are Most at Risk
Certain cancer treatments increase risk for osteoporosis. The men most at risk have:
- Low testosterone as a result of cancer treatment.
- Prostate cancer that is treated with androgen deprivation therapy (also called hormone therapy or androgen suppression therapy). These therapies include:
- orchiectomy (surgery to remove the testicles)
- luteinizing hormone-releasing hormone (LHRH) agonists, such as leuprolide (Lupron®, Eligard®), goserelin (Zoladex®), triptorelin (Trelastar®) and histerelin (Vantas®)
- LHRS agonists such as degarelix (Firmagon®)
- the CYP17 inhibitor abiraterone (Zytiga®)
- the hormone blocker ketoconazole (Nizoral®)
If you are on these treatments, it will be important to have bone density tests every two years, take calcium and vitamin D supplements, and talk to your doctor about whether to take a bone-building drug.
Other Cancer Treatments that Increase Risk
These cancer treatments also increase risk for bone loss in women and men:
- Radiation to weight bearing bones (spine, hips, legs). Radiation weakens the bone and can cause osteoporosis by damaging osteoblasts and osteoclasts.
- Allogenic (receiving a donor’s) stem cell and bone marrow transplants.
- Steroids known as glucocorticoids, such as prednisone, prednisolone, dexamethasone, and cortisone.
- Surgical removal of the stomach (gastrectomy).
Survivors of childhood cancers are also at higher risk of developing osteoporosis.
Keeping Your Bones Healthy
It is important for people who have been treated for cancer to do things to help maintain bone density. If you started taking medicine to treat osteoporosis before your cancer diagnosis, you can still take steps to keep your bones healthy. These include:
- Not smoking—it makes bone loss happen faster
- Limiting alcohol to one drink a day (for women) or two (for men)
- Eating a diet rich in calcium and vitamin D
- Exercising
- Preventing falls
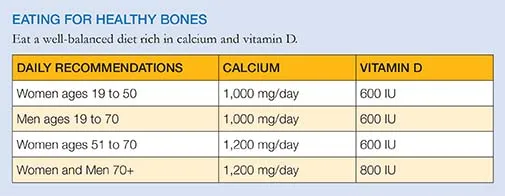
Calcium and Vitamin D
Try to get your daily recommended levels of calcium and vitamin D from the food you eat. Good sources of calcium include:
- Low-fat dairy products, like yogurt
- Kale and other dark green, leafy vegetables like spinach, collard greens, turnip greens, and bok choy (a kind of Chinese cabbage)
- Broccoli, acorn squash, butternut squash, and okra
- Canned salmon or sardines with bones
- Calcium-fortified foods and drinks (orange juice, soy milk, almond milk, some cereals, breads, and tofu are often fortified with calcium and vitamin D)
- Figs, dried fruit, and almonds
- Beans and peas, especially soybeans and black eyed peas
Talk to your health care provider about whether calcium and vitamin D supplements are right for you.
Exercise for Bone Health
Exercise is a key part of a healthy lifestyle that helps maintain bone density. Exercise:
- Improves balance, which makes you less likely to fall
- Lowers your risk of heart disease and blood clots
- Can help you maintain a healthy weight. This helps reduce your risk of having your cancer come back (recur). It also reduces your risk of heart disease.
During and after your cancer treatment, you may not have as much energy or flexibility as you had before you started treatment. Even so, you should try to move as much as you can. Talk to your doctor about what types of exercises are okay for you now.
Exercise Tips
- Try to build up to 30 minutes each day.
- Do things that feel good and safe, like walking with friends, gardening, swimming or gentle yoga.
- Try to add in some resistance exercises, like lifting weights and stretching with exercise bands. This builds muscle strength, which helps support your bones.
- When you feel sick, exercise only as much or as strenuously as you feel comfortable.
- Allow yourself to exercise gently, slowly, and for short amounts of time.
- If you are very tired, try gentle, slow, and brief movements that are comfortable. You can do more on a day you are not as tired.
- If you have trouble sleeping, exercise during the day to help you sleep better at night.
Prevent Falls
Thin bones are more likely to break if you fall. To prevent falls, you can:
- Wear low-heeled shoes that fit well.
- Get shoes with nonslip soles.
- Check your house—move anything you could easily trip over (electrical cords) or slip on (rugs).
- Keep rooms brightly lit.
- Put grab bars inside and outside your bath or shower (and ask for rooms that have them when you are staying at a hotel).
- Lower your mattress if it is hard for you to get out of bed.
- Consider buying a pair of walking sticks, especially if walking or hiking is your favorite type of exercise.
- Talk to your doctor about whether you should start a strength-training program. This could be a pool exercise program or involve using resistance from weights or bands.
Other Treatments for Osteoporosis
Eating a healthy diet, exercising, preventing falls, and taking bone-building drugs (if you need them) can help keep your bones strong, reduce your risk of broken bones, and improve your well-being.
Treatment with Bone Building Drugs
If you are diagnosed with osteoporosis, your doctor will recommend that you take bone building drugs to help reduce your risk of broken bones. (You may already be on an osteoporosis drug at the time of your cancer diagnosis.)
Bisphosphonates
The drugs most often used to treat osteoporosis are called bisphosphonates (bis-FOS-foy-nayts). They include:
- alendronate (Fosamax®)
- risedronate (Actonel®)
- ibandronate (Boniva®)
- zoledronate (Zometa®, Reclast®).
Some are taken by mouth (oral). Others are given by IV (into your vein).
- Oral drug side effects include: nausea, abdominal pain and heartburn like symptoms.
- IV drug side effects include: fever, headache, and muscle aches for up to three days.
Ask your doctor:
- Which drugs does my insurance cover?
- Is there a patient assistance program that can help cover all or part of the cost?
Rare complications include:
- Developing a crack in the middle of the thigh bone after being on them for more than five years.
- Osteonecrosis (bone death) of the jaw after having a tooth pulled. For this reason, you should have a dental exam before starting.
Other Bone Building Drugs
Raloxifene (Evista®) for Women
Evista is a pill used to reduce breast cancer risk in women at high risk for the disease. But, it is also used to treat osteoporosis in women after menopause. Its side effects include hot flashes and increased risk of blood clots.
Depending on the type of cancer treatment you are receiving, your doctor may recommend one of these bone-building drugs:
- denosumab (Prolia®), a shot given every six months. It is used to reduce bone loss in women on an aromatase inhibitor and men on a treatment that suppresses testosterone.
- teriparatide (Forteo®), a shot given daily. After two years of treatment with Forteo, another osteoporosis drug is given to maintain the new bone growth.